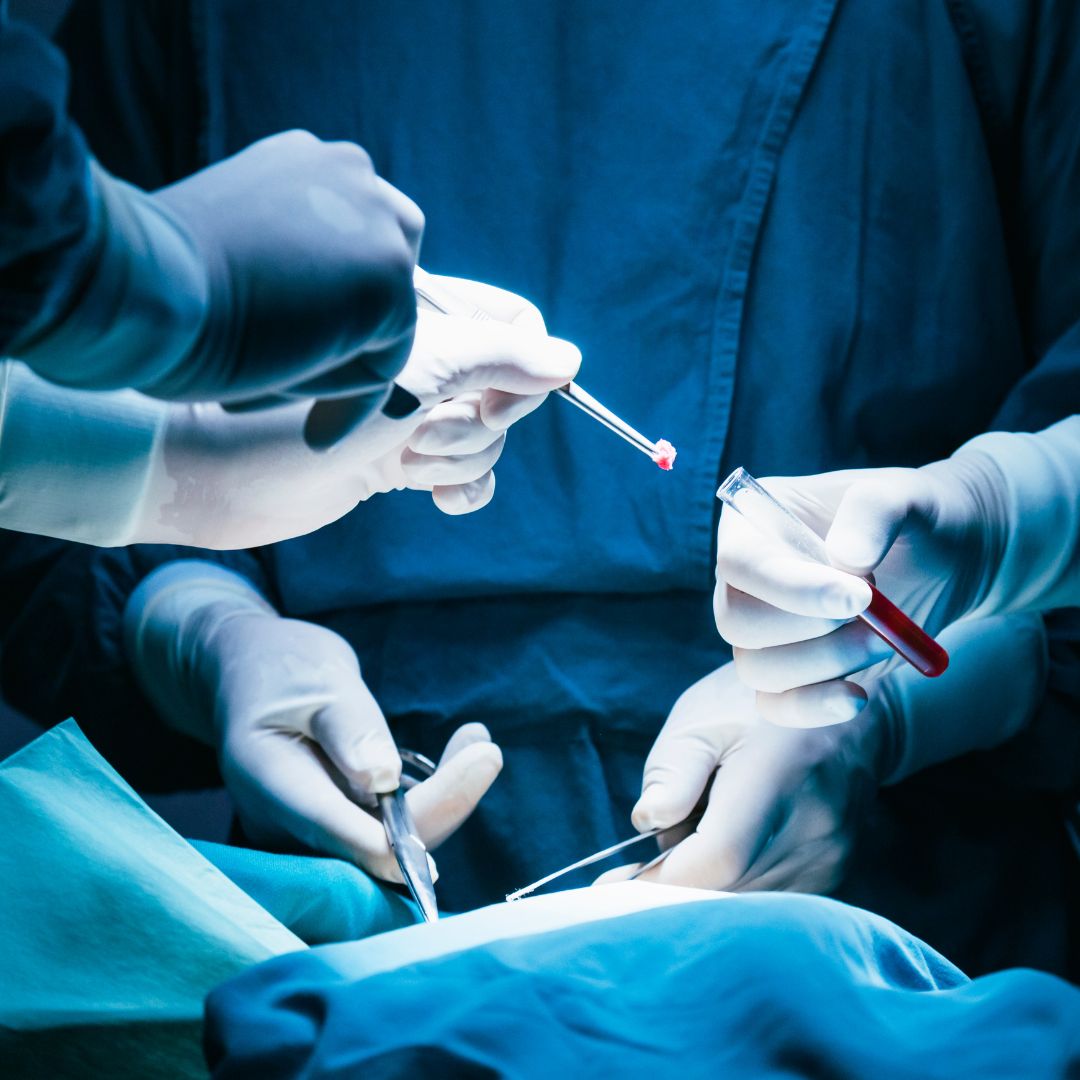
When a surgical specimen goes missing or is mislabeled, cases stall, re-collections follow, and confidence erodes. In the operating room, minutes are compressed and handoffs are frequent. Barcode labels help at single touchpoints, but they do not show what happens between them.
OR specimen tracking requires visibility across every transition, not just confirmation at pickup and receipt. Passive RFID closes these gaps by automatically recording specimen movement and giving teams a fast, reliable way to recover off-route items. This article outlines a practical hospital specimen tracking model that health systems can standardize across operating rooms and pathology workflows.
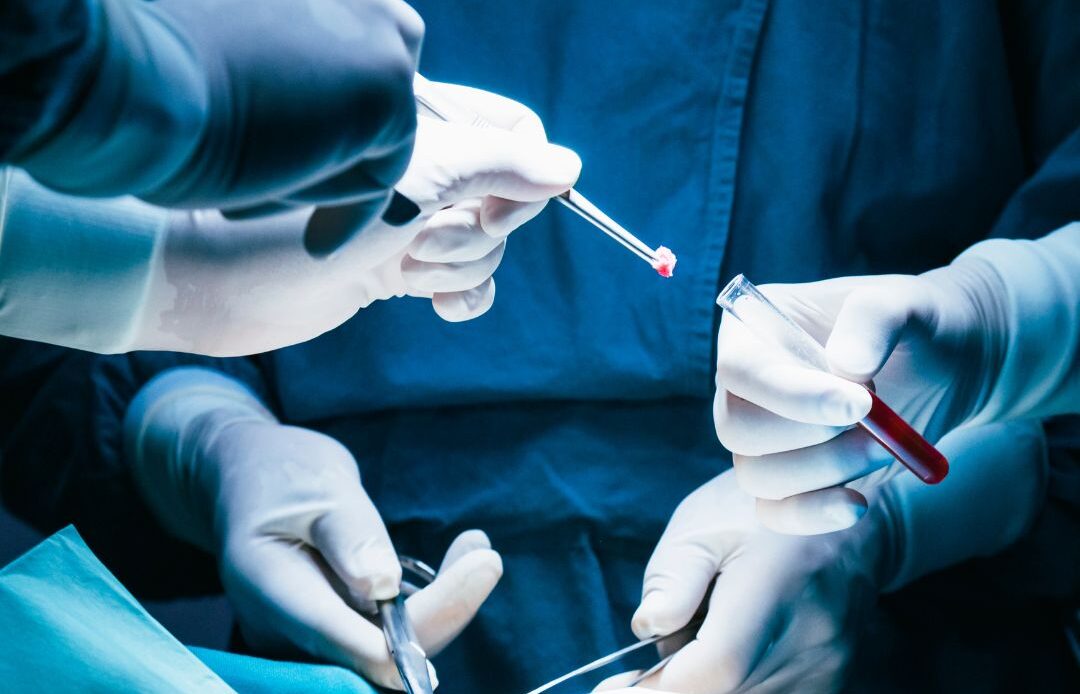
What Breaks in OR Specimen Tracking Today
Specimen tracking in the OR breaks down for predictable reasons. Look-alike containers, rapid handoffs, and competing priorities make manual logs unreliable. A specimen can move from the sterile field to a pass-through, to dispatch, to courier pickup, and to lab receiving in minutes.
When even one step is missed, the trail goes cold. Staff are forced into time-consuming searches or repeat collections. The goal of hospital specimen tracking should be simple: create a searchable chain of custody from the OR to accessioning in Histology or Cytology without adding new steps for clinical teams.
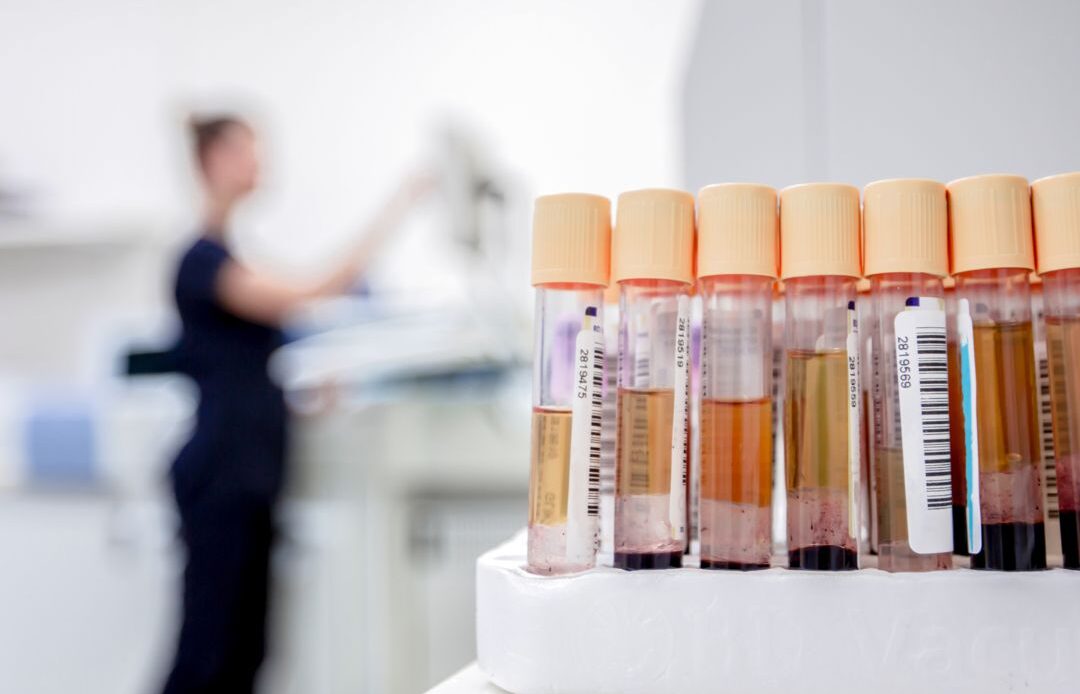
RFID Specimen Tracking in The OR: How It Works in Practice
OR specimen tracking with RFID begins at label printing. At that moment, the specimen container also receives a passive RFID tag carrying a non-PHI identifier linked to the LIS order.
From there, fixed RFID readers do the work in the background. Placed at natural transition points such as OR core doors, pass-through windows, specimen dispatch desks, unit exits, and lab receiving thresholds, these readers automatically record time and location events as specimens move.
Staff continue to work as they always have. The system quietly builds a complete custody record without relying on manual scans or log entries.
When a specimen is not where it should be, recovery is straightforward. Teams check the last observed location and use a handheld RFID reader to perform a proximity search. Signal strength increases and audible cues guide staff directly to the shelf, cart, or cooler where the specimen resides, often within minutes.
For refrigerated or frozen specimens, temperature data loggers can record pass or fail status alongside custody events, supporting quality standards and accreditation requirements.
Read Zones That Map to Real OR And Lab Flow
Every hospital is different, but effective hospital specimen tracking follows consistent movement patterns.
- •OR thresholds or pass-through windows capture the moment a specimen leaves the room
- •Specimen dispatch desks or tube stations confirm consolidation before courier pickup
- •Unit exits or courier handoff points initiate expected-arrival timing
- •Lab receiving thresholds confirm arrival and reconcile expected versus received specimens by LIS order
- •Cold rooms and freezers provide zone-level presence until processing in Histology or Cytology
These placements reflect how specimens actually move through the organization. They remove manual steps while increasing reliability and auditability.
What Hospitals and IDNs Gain from OR Specimen Tracking
Hospitals implementing RFID-based specimen tracking in the OR see measurable operational and clinical benefits.
Search time drops dramatically, reducing delays and re-collections. OR teams avoid unnecessary re-sterilization cycles tied to specimen uncertainty. Pathology receives specimens with a complete, defensible chain of custody.
Quality and compliance teams gain a single source of truth for time, location, and temperature where required. Leaders gain visibility into where handoffs break down and where automation removes risk.
Most importantly, the approach is staff friendly. Fixed readers automate routine events. Handhelds are used only for exceptions. This aligns with broader healthcare trends toward passive data capture, reduced cognitive load, and fewer workarounds, all priorities highlighted in the Zebra Technologies Healthcare Vision Study.
Example End-To-End OR Specimen Tracking Workflow
A case begins and the specimen label and RFID tag are printed together. The sealed container leaves the sterile field and a fixed reader records exit from the OR core. Dispatch confirms pickup. Lab receiving logs arrival and reads tags inside the bag or cooler, matching them to expected LIS orders.
Accessioning follows, with storage status recorded until processing in Histology or Cytology. If anything does not match, staff initiate a proximity search from the last observed location and resolve the exception quickly, before delays escalate.
What to Measure: KPIs That Matter
Hospitals evaluating OR specimen tracking should monitor:
- Lost or delayed specimens per 10,000 orders
- Median time to locate an off-route specimen
- Percentage of LIS orders with a complete custody trail from OR to accessioning
- Re-collections and patient call backs
- Cold-chain exceptions for refrigerated or frozen specimens
- Receiving auto-match rate and time to resolve exceptions
Implementation Notes For Multi-Site Hospital Networks
IDNs achieve the best results by establishing a standard specimen tracking model and rolling it out in phases. Many start with a receiving portal and handheld recovery on a high-volume route. As volume grows, exit portals are added at busy OR cores to remove manual steps.
Label policies, read-zone placement, dashboards, and alerts are then standardized across hospitals. Integrations pass custody events to the LIS through interface engines or approved APIs. Data retention and access controls align with CAP and Joint Commission requirements.
See OR Specimen Tracking in Action
Schedule an in-person or remote demo for your OR, Pathology, and operational leadership. Call (425) 438-2533 or contact us online. Visit our Healthcare Resources hub or explore additional guidance on preventing specimen mix-ups with RFID-based chain of custody for Pathology, Histology, and Cytology.